Development of the eye
The eyes begin to develop either side of the
developing forebrain as optic vesicles by the end of fourth week. Continuous
with the forebrain the optic vesicles contact the surface ectoderm and induce
development of the lens placode. When the optic vesicle invaginates to form the
pigmented and neural layers of the retina, the lens placode also invaginates
forming the lens pit and lens vesicle.
The retina, optic nerve, muscles and epithelium
of the iris, and ciliary body are all derived from the neuroectoderm of the
forebrain, while the lens and epithelium of the lacrimal glands, eyelids,
conjunctiva and cornea all arise from the surface ectoderm. The extraocular
muscles and all of the connective and vascular tissue of the cornea, iris,
ciliary body, choroids and sclera are of mesodermal origin.
The eyeball
The eyeball consists of three concentric
layers, an outer fibrous supporting layer comprising the sclera and cornea; a
middle vascular, pigmented layer comprising the choroids, ciliary body and
iris; and an inner layer of nerve elements, the retina. The interior of the
eyeball contains fluid under pressure and is divided into anterior and
posterior compartments, containing aqueous humour and the vitreous body
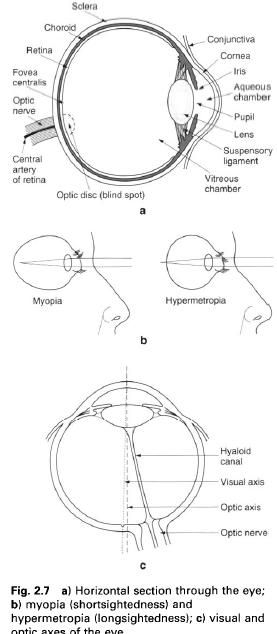
respectively, by the lens and its attachments(figure a).
A thin fibrous sheet surrounds the sclera
forming a socket for the eyeball and separating it from the other contents of
the orbit. The eyeball is supported inferiorly by the suspensory ligament, and
surrounded and protected by extraocular fat. In adults the eyeball is almost
spherical, having a diameter of 25mm; however, the anteroposterior diameter may
be greater or less than normal giving rise to myopia(short – sightedness) or hypermetropia(long
– sightedness) respectively(figure b). Relative to body size the eyeball is
much larger in infants and children since it completes the majority of its
growth in the antenatal period: it is also slightly larger in women than in
men.
The two eyes look forwards and an imaginary
line connecting the centre of the corneal curvature(the anterior pole) to the
centre of the scleral curvature(the posterior pole) is known as the optic
axis(figure c). The visual axis is, however of more importance and joins the
centre of the cornea to the fovea of the retina, and represents the course
taken by light from the centre point of vision. When looking at distant objects
the visual axes of the two eyes are parallel, the optic axes are slightly and
the optic nerves markedly convergent posteriorly.
Outer fibrous layer
The sclera is the posterior opaque part of the
fibrous layer and forms about five-sixths of the circumference of the eyeball,
the remainder being cornea. It is 1mm thick posteriorly and 0,5mm thick
anteriorly and has the tendons of the extraocular muscles attaching to it. The
anterior part of the sclera is covered by conjunctiva and forms the “white of
the eye”. Posteriorly the sclera is pierced, 3mm medial to the fovea, by the
optic nerve and accompanying vessels(figure a).
The forward – bulging cornea is continuous with
the sclera at the corneoscleral junction. It is dense and uniformly 1mm thick,
being covered by conjunctiva. The cornea is avascular but richly innervated by
the ophthalmic nerve with abrasions being extremely painful: its sensitivity to
touch forms the basis of the corneal reflex which results in reflex contraction
of orbicularis oculi and closure of the eye.
The majority of the refraction of the eye takes
place at the surface of the cornea and not at the lens. Irregularities in the
curvature of the cornea, which ideally should correspond to a section of a
perfect sphere, interfere with the ability to form sharp images on the retina.
When the cornea is more curved in one direction than the other the condition is
known as astigmatism.
The surface conjunctiva and cornea are kept
moist and clean by a watery fluid secreted by the lacrimal gland. Constant
blinking is an important part of the mechanism of fluid flow across the cornea:
drying of the cornea causes serious damage to its surface cells.
Middle vascular layer
This is often called the uvea and consists of
three parts, the choroids, the ciliary
body and the iris(figure a). The chorioid is a thin membrane lining the
sclera as far as the corneoscleral junction, being loosely connected to the
sclera except near where the optic nerve pierces when it is firmly attached. It
consists of two parts, an outer pigmented(brown) layer, which prevents light
passing through the sclera and the scattering of light which enters via the
pupil, and an inner vascular layer which is nutritive to the outer layer of the
retina.
The ciliary body is a wedge-shaped ring
connecting the choroids to the iris, and contains the ciliary muscle and
ciliary processes, being lined by the ciliary part of the retina(figure a). The
inwardly projecting part of the wedge is directed towards the lens, being
connected to it by fibres of the suspensory ligament of the lens. The ciliary
muscle consists of two sets of smooth muscle fibres: an inner oblique set and
an outer radial set, with both sets being under parasympathetic control.
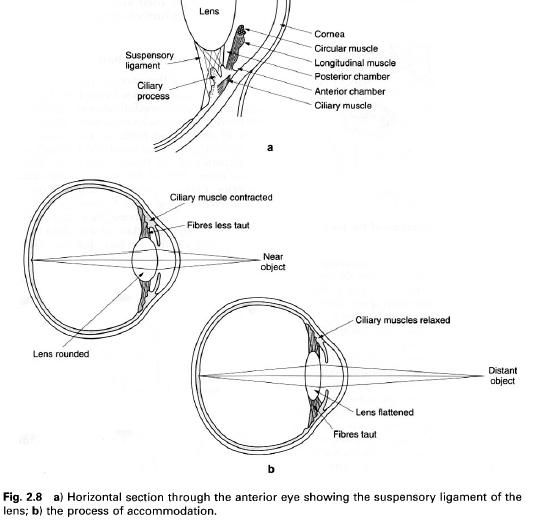
Contraction of the ciliary muscle reduces tension in the suspensory ligament of
the lens allowing its natural elasticity to increase its curvature so that the
eye can focus on near objects, the process of accommodation. The ciliary
processes are sixty to eightly radiating projections, 2mm is length, and also
give attachment to the suspensory ligament of the lens.
The iris is a thin contractile membrane, firmly
attached at its periphery to the ciliary body, lying in front o the lens with a
central opening, the pupil. It contains smooth muscle fibres organized into an
inner circular sphincter pupilla and an outer radially arranged dilator
pupilla. These two muscles control the size of the pupil and thus the amount of
light entering the eye. Both muscles are under autonomic control, the sphincter
pupillae being parasympathetic and the dilator pupillae sympathetic. The colour
of the iris is due to pigment cells in its posterior layer. In individuals with
few pigment cells, and because of the way other elements of the iris absorb and
reflect light, the iris appears pale blue; with increasing numbers of pigment
cells the iris darkens and may become dark brown.
Refracting media
The iris partly divides the region in front of
the lens into anterior and posterior chambers, both of which contain aqueous
humour(figure 1a). This is clearly watery solution formed by the epithelium of
the ciliary processes: the fluid is resorbed at the iridocorneal angle into the
sinus venosus to re-enter the circulation. Interference with the process of
resorption results in an increased intraocular pressure, glaucoma, which
affects the peripheral part of the visual field due to pressure on the retina.
Behind the lens and ciliary body is the vitreous body, a transparent,
colourless semigelatinous material(figure 1a).
The lens is biconvex, 10mm in diameter and 4mm
thick, becoming thinner in old age. It
largely consists of concentric lamellae of lens fibres surrounded by a
capsule which is firmly attached to the ciliary body by the suspensory ligament
of the lens. Both the capsule and lens are transparent and elastic. The shape
of the lens is modified by the ciliary muscle as the eye focuses on objects at
different distances(figure 2b). After middle age the lens becomes less elastic
and the ability to accommodate is gradually lost(presbyopia), so that glasses are required for close work. The lens
may also become less transparent with increasing age, giving rise to cataract.
Inner nervous layer
The inner layer is the light sensitive layer,
more commonly known as the retina, and extends onto the ciliary body and iris
but in this region contains no nerve elements so is non-functioning. The retina
is 0.5mm thick posteriorly thinning to 0.1mm anteriorly; however, both the
optic disc and the fovea centralis are much thinner areas. It comprises two
parts, an outer pigmented epithelial layer and an inner transparent layer
containing the light receptors(rods and cones)(figure below). The region where
the fibres forming the optic nerve converge to pass through the choroids and
sclera is the optic disc. It contains no light receptors and is therefore
insensitive to light(the blind spot).
3mm lateral to the optic disc is the macula, which has at its centre a
depression, the fovea centralis, where vision is most acute(figure 1a).
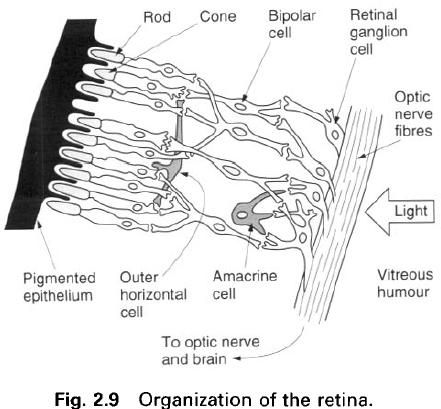
Within the inner transparent layer the rods and
cones lie closest to the choroids, so that light has to pass through most of
the retina before reaching them(figure up). The cones are used in bright light
as well as for colour discrimination. The macula contains only cones so that it
functions in detailed vision, i.e. when an object is specifically looked as it
is always focused on the macula. From the macula outwards the number of cones
rapidly decreases, however the number of rods increases; the rods are used in
dim light. The pigment contained in the rods is bleached out in bright light
but reforms in dim light so that objects previously not visible are seen(dark
adaptation). There are six times as many rods as cones in the retina.
The blood
supply to the retina is essentially from the central artery of the retina, a
branch of the ophthalmic artery, which divides into four branches each supplying
a separate quadrant of the retina. Because each of these branches is an
end-artery, blockage results iin blindness in the appropriate quadrant. The
retina may also become detached from the choroids, either spontaneously or as a
result of a blow to the eye, and vision is impaired. If the retina is torn
fluid passes outside the layer of rods and cones with vision again being lost.
In both cases laser treatment can be used to reattach the retina in order to
prevent further separation.
Movements of the eyeball
The direction of the gaze is controlled by the
extraocular muscles, these being the four rectus muscles(superior, medial,
inferior, lateral) and the two oblique muscles(superior, inferior). The recti
all attach posteriorly to a tendinous ring surrounding the optic canal and
medial part of the superior orbital fissure, and insert into the sclera 6mm
behind the edge of the cornea. Superior oblique passes forwards from the medial
wall of the orbit to hook around the trochlea on the frontal bone, then backwards
to attach to the upper surface of the sclera behind the equator of the eyeball.
Inferior oblique passes laterally from the medial part of the maxilla below
inferior rectus to attach to the sclera, again behind the equator of the
eyeball. Of these muscles lateral rectus is innervated by the abducens(VI)
nerve, superior oblique by the trochlear(IV) nerve and the remainder by the
oculomotor(III) nerve.
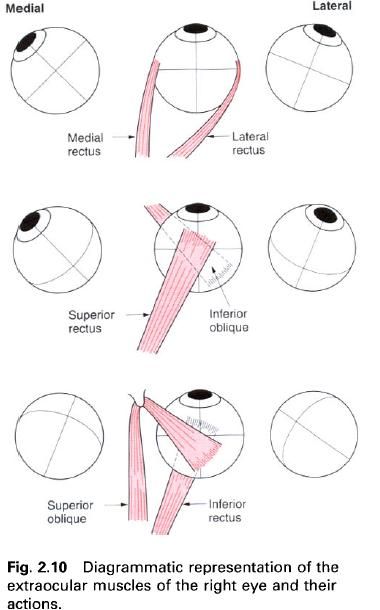
The medial and lateral rectus turn the eye to
look horizontally, medially and laterally respectively(figure below). However,
because of the oblique course of the superior and inferior rectus within the
orbit they tend to pull the eye medially in addition to turning it to look up
and down respectively(figure below). The two oblique muscles on the other hand
tend to pull the eye laterally as well as moving it up and down(figure below).
Because the obliques attach behind the equator they pull on the back of the
eyeball. Consequently superior oblique turns the eye to look downwards and
laterally, while inferior oblique turns it to look upwards and laterally. In
reality almost every movement of the eyeball involves at least three muscles.
Coordinated movement between the two eyes is controlled by the brain.









0 коментара:
Постави коментар