Cardiovascular function
Exercise increases the demands of the
cardiovascular system. When the need to regulate body temperature is added
during exercise in the heat, the cardiovascular system can become burdened.
During exercise in hot conditions, the circulatory system has to continue to transport
blood not only to working muscle but
also to the skin, where the heat generated by the muscles can be transferred to
the environment. To meet this dual demand during exercise in the heat, two
changes occur. First, cardiac output increases
further(above that associated with a similar exercise intensity in cool
conditions) by increasing both heart rate and contractility. Second, blood flow is shunted away from
nonessential areas like the gut, liver, and kidneys and to the skin.
Consider what happens during running at a fast
pace on a hot day. The exercise increases both metabolic heat production and
the demand for blood flow and oxygen
delivery to the muscles. This excess heat can be dissipated only if blood flow increases to the skin.
As the thermoregulatory center instructs the
cardiovascular system to direct more
blood flow to the skin, superficial blood vessels dilate to bring more of
the warm blood to the body’s surface.
Sympathetic nervous system signals also go to the heart to increase heart rate and allow the left ventricle
to pump more forcefully. The gradual upward drift in heart rate helps compensate for the decrease in stroke volume as blood pools in the periphery. This phenomenon is known as cardiovascular
drift. Because blood volume stays constant or even decreases some(as
fluid is lost in sweat), a final phase of cardiovascular adjustment occurs.
Sympathetic signals to the kidneys, liver, and intestines cause
vasoconstriction of those regional circulations, which allows more of the available
cardiac output to reach the skin
without compromising muscle blood flow.
What limits exercise in the heat?
Seldom are records set in endurance events,
such as distance running, when the environmental heat stress is great. The
factors that cause early fatique when heat stress is superimposed on prolonged
exercise have been the topic of some debate, and several theories have been
proposed. None of these theories captures every situation, but taken together
they demonstrate the multiple control systems at work during thermoregulation.
At some point, the cardiovascular system can no longer compensate for the increasing
demands of continuing endurance exercise and efficiently regulating the body’s
heat. Consequently, any factor that tends to overload the cardiovascular system or to interfere with heat dissipation can
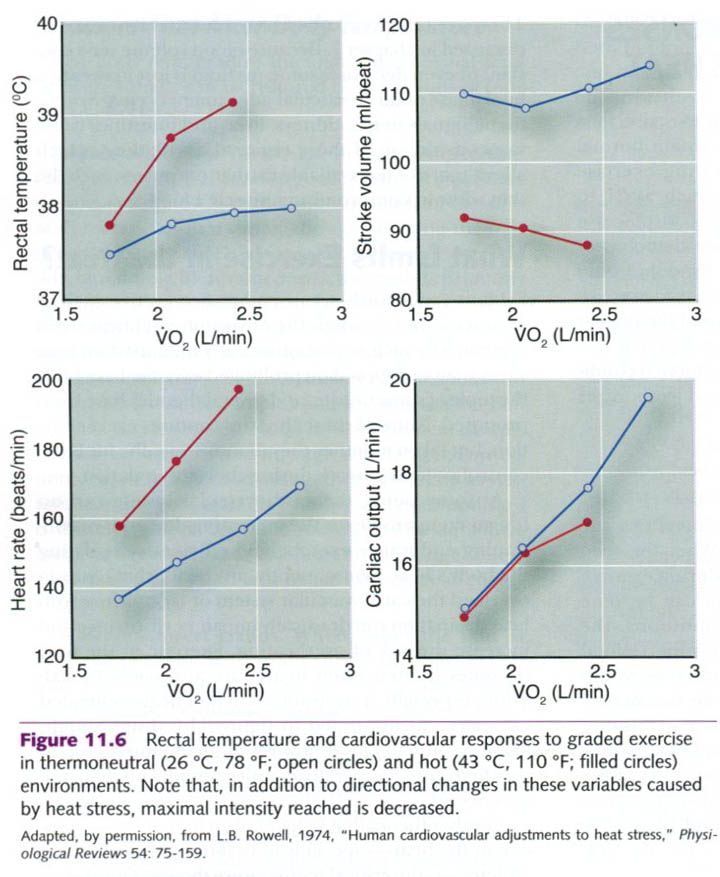
drastically impair performance and increase the risk of overheating. Exercise
in the heat becomes limited when heart rate approaches maximum, especially in
untrained or non-heat-acclimated exercisers, as illustrated in the figure
below. Interestingly, working muscle blood flow is well maintained even at very high core temperatures unless
significant dehydration occurs.
Another theory that helps explain limitations
to exercise in the heat – especially in well-trained, acclimated athletes – is
the critical temperature theory.
This theory proposes that, regardless of the rate at which core temperature(and
thus brain temperature) increases, the brain will send signals to stop exercise
when some critical temperature is reached, usually between 40 and 41°C(104 and
105.8°F).
Body fluid balance
Under some conditions, the temperature of the
environment approaches and can exceed both the skin and deep body temperatures.
As mentioned earlier, this makes evaporation far more important for heat loss,
because radiation, convection, and conduction become increasingly less effective is environmental temperature
increases. In fact, these mechanism lead to heat gain when environmental
temperature exceeds skin temperature. Increased dependence on evaporation means
an increased demand for sweating.
The sweat glands are controlled by stimulation
of the POAH. Elevated blood
temperature causes this region of the hypothalamus to transmit impulses through
the sympathetic nerve fibers to the millions of eccrine sweat glands
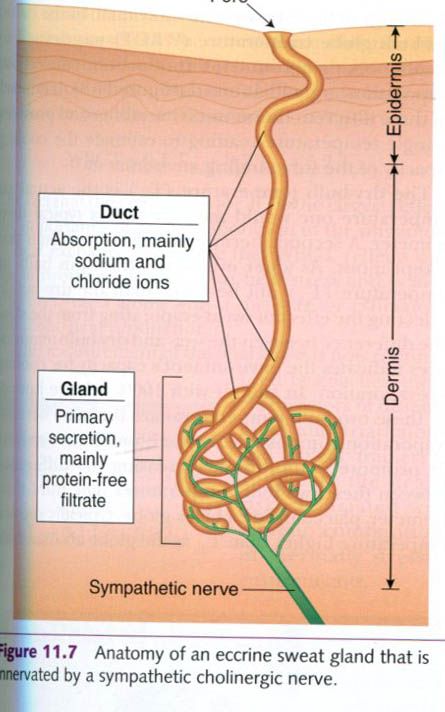
distributed over the body’s surface. The sweat glands are fairly simple tubular
structures extending through the dermis and epidermis, opening onto the skin,
as illustrated in the picture below.
Sweat is formed in the coiled secretory portion
of the sweat gland and at this stage has an electrolyte content similar to that
of the blood, since plasma is the
source of sweat formation. As this filtrate of plasma passes through the
uncoiled duct of the gland, sodium and chloride are reabsorbed back into the
surrounding tissues and then into the blood.
As a result, the final sweat that is extruded onto the skin surface through the
sweat gland pores is hypotonic to(has less electrolytes than) plasma. During
light sweating, the filtrate sweat travels slowly enough through the duct that
there is time for reabsorption of sodium and chloride. Thus, the sweat that
forms during light sweating contains very little of these electrolytes by the
time it reaches the skin. However, when the sweating rate increases during
exercise, the filtrate moves more quickly through the tubules, allowing less
time for reabsorption, and the sodium and chloride content of sweat can be
considerably higher.
Example
of sodium, chloride, potassium
concentrations in the sweat of trained and untrained subjects during exercise
|
|||
Subjects
|
Sweat
Na+(mmol/L)
|
Sweat
Cl-(mmol/L)
|
Sweat
K+(mmol/L)
|
Untrained
men
|
90
|
60
|
4
|
Trained
men
|
35
|
30
|
4
|
Untrained
women
|
105
|
98
|
4
|
Trained women
|
62
|
47
|
4
|
As seen in the table up, the electrolyte
concentration of trained and untrained subjects sweat is significantly
different. With training and repeated heat exposure(acclimation), more sodium
is reabsorbed and the sweat is more dilute, in part because the sweat glands
become more sensitive to the hormone aldosterone.
Unfortunately, the sweat glands apparently do not have a similar mechanism for
conserving other electrolytes. Potassium,
calcium, and magnesium are not reabsorbed by the sweat glands and are therefore
found in similar concentrations in both sweat and plasma. In addition to heat
acclimation and aerobic training, genetics is a major determinant of both
sweating rate and sweat sodium losses.
While performing heavy exercise in hot
conditions, the body can lose more than 1L of sweat per hour per square meter
of body surface. This means that during intense effort on a hot and humid
day(high level of heat stress), an average-sized individual(50-75kg, or
110-165lb) might lose 1.6 to 2.0L of sweat, or about 2.5% to 3.2% of body
weight, each hour. A person can lose a critical amount of body water in only a
few hours of exercise in these conditions.
A high rate of sweating maintained for a
prolonged time ultimately reduces blood volume. This limits the volume of blood
returning to the heart, increasing heart rate and ultimately decreasing cardiac output, which in turn reduces
performance potential, particularly for endurance activities. In long-distance
runners, sweat losses can approach 6% to 10% of body weight. Such severe
dehydration can limit subsequent sweating and make the individual susceptible
to heat-related illnesses.
Loss of both electrolytes and water in the
sweat triggers the release of both aldosterone
and antidiuretic hormone(ADH),
also know as vasopressin or arginine vasopressin. Aldosterone is
responsible for maintaining appropriate sodium levels and ADH maintains fluid balance. Aldosterone is
released from the adrenal cortex in response to stimuli such as decreased blood
sodium content, reduced blood volume, or reduced blood pressure. During acute
exercise in the heat, this hormone limits sodium excretion from the kidneys.
More sodium is retained by the body, which in turn promotes water retention.
Because of this, plasma and interstitial fluid volumes can increase 10% to 15%.
This allows the body to retain water and sodium in preparation for additional
exposures to the heat and subsequent sweat losses.
Similarly, exercise and body water loss
stimulate the posterior pituitary gland
to release ADH. This hormone stimulates water reabsorption from the kidneys,
which further promotes fluid retention in the body. Thus, the body attempts to
compensate for loss of minerals and water during periods of heat stress and
heavy sweating by reducing their loss in urine. Also, blood flow to the kidneys
is substantially reduced during exercise in the heat, which aids in fluid
retention during acute bouts of exercise.









0 коментара:
Постави коментар